Obsessive Compulsive Disorder (OCD) is a crippling and serious mental health condition, characterised by unwanted, persistent thoughts (obsessions) and repetitive behaviours (compulsions). It is deeply distressing cycles that can quietly affect daily functioning. For many individuals, the struggle is not just with the thoughts themselves, but with the urge to respond to them in ways that feel temporarily relieving, yet ultimately reinforcing.
In this post, we’ll explore what exactly OCD is and how CBT disrupts the obsessive compulsive cycle.
The Cycle of Obsessive Compulsive Disorder (OCD)
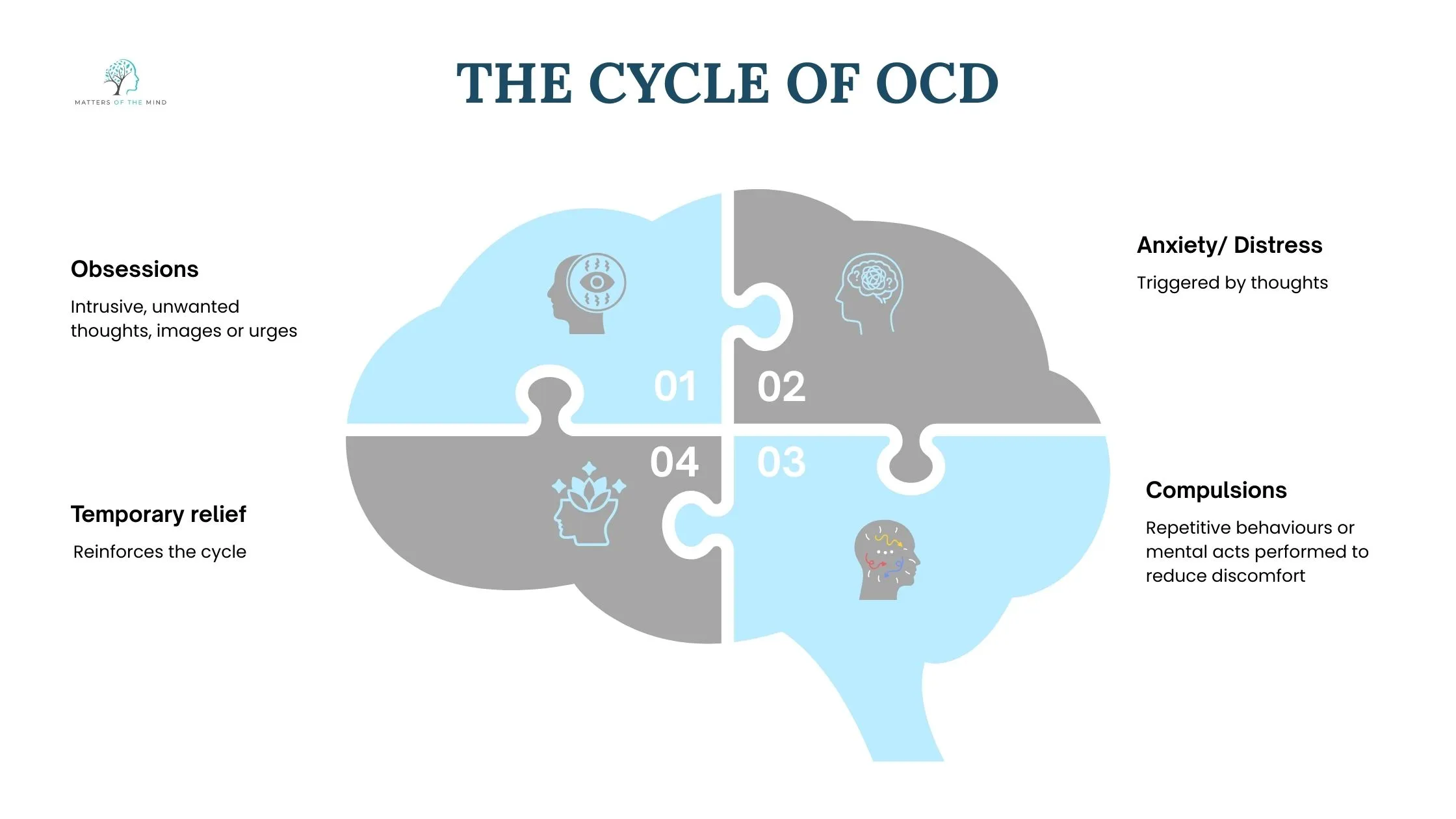
If OCD can be deeply analysed, it operates in a loop:
- Obsessions: intrusive, unwanted thoughts, images or urges
- Anxiety or distress triggered by thoughts
- Compulsions: repetitive behaviours or mental acts performed to reduce discomfort
- Temporary relief, which reinforces the cycle
Over time, this loop becomes automatic. The more the compulsions are performed, the stronger the brain associates them with relief, making the cycle harder to break. This is the reason why OCD treatment requires more than just managing symptoms; it requires addressing the pattern, too.
Common OCD Symptoms
OCD involves the listed symptoms that affect overall functioning. It typically includes:
- Persistent fear of harm
- Repeated checking
- Excessive cleaning or washing
- Intrusive thoughts that feel difficult to control
- Mental habits such as reassurance seeking or validation
These symptoms are not simply habits; they are coping responses driven by anxiety. They not only ensure mental discomfort, but also unintentionally strengthen the obsessive patterns over time.
What is Cognitive Behavioural Therapy for OCD?
Cognitive behavioural therapy for OCD is a structured, evidence-based approach that focuses on how thoughts, emotions, and behaviours are interconnected. CBT aims to help individuals identify and recognise the distorted thinking patterns that contribute to their compulsive behaviours.
CBT operates on the premise that changing unnecessary thought patterns can lead to changes in behaviour and emotional responses. For individuals with OCD, this means challenging the irrational beliefs that fuel obsessions and compulsions, thereby reducing the associated stress and anxiety.
Rather than eliminating the thoughts, CBT for OCD works on changing the way thoughts are interpreted, reducing the emotional impact of obsessions, and gradually modifying behavioural responses.
One of the most effective components of CBT therapy for OCD is Exposure and Response Prevention (ERP), widely considered the gold standard approach.
How does CBT help OCD? Breaking the Vicious Loop

1. Changing the meaning of thoughts
In obsessive-compulsive disorder, thoughts are misinterpreted as dangerous or significant.
CBT helps individuals recognise that thoughts are not actions, that having a thought does not make it true, and that uncertainty can be tolerated. This shift reduces the urgency to neutralise thoughts through compulsions.
2. Reduce fear sensitivity
A key part of CBT for OCD involves gradually facing feared situations or thoughts in a controlled or supportive way. Instead of avoiding triggers, individuals learn to approach them. For example, touching a surface without immediately washing hands, or leaving a task unchecked despite discomfort.
This process gives exposure, and it helps reduce the fear over time by teaching the brain that the perceived threat is not as dangerous as it feels.
3. Response prevention
If treating OCD with CBT is necessary, it is equally important to learn not to perform compulsive behaviours after the anxiety is triggered. This step may feel uncomfortable initially, but it is where real change begins. When compulsions are resisted, anxiety rises temporarily and then naturally decreases on its own. Over repeated practice, the brain learns that compulsions are not necessary for relief.
4. Rewriting the brain’s learning pattern
OCD is maintained by reinforcement, with compulsions working in the short term, so the brain keeps using them. However, CBT interrupts this pattern. Research shows that exposure-based CBT leads to a significant reduction in symptom severity, as individuals begin to experience that feared outcomes often do not occur. This process is often known as habituation (anxiety reduces with repeated exposures) or cognitive restructuring (changing belief patterns).
What makes CBT Effective for OCD Treatment?
CBT is considered one of the most effective approaches for OCD therapy because it:
Addresses both thought patterns and behaviours
Encourage self-awareness and mindfulness
Provide practical, structured tools
Focus on long-term change
Studies have shown that a significant number of individuals have seen noticeable changes and a reduction in OCD symptoms, with substantial recovery.
Move Forward
You don’t have to stay stuck in the OCD cycle. Take the first step towards lasting change today.
Final Thoughts
Obsessive-compulsive disorder (OCD) can feel like an unending loop, but it is not a fixed one. OCD treatment is not about eliminating thoughts; it is about responding differently, reducing fear over time, and regaining a sense of control. There may be moments of discomfort during the process, but these moments are often where the most meaningful change begins.
Through cognitive behavioural therapy (CBT), individuals are not taught to fight their thoughts, but to relate them differently. With consistent guidance and practice, the cycle of obsession and compulsion begins to loosen, making space for a more balanced and manageable way of living.
Dr Kavita Deepak-Knights offers a personalised approach to OCD therapy, focusing on evidence-based techniques like CBT for OCD to support long-term change at a pace that feels manageable.
Taking the first step can make all the difference. Book a personalised session with Dr Kavita Deepak-Knights and take the first step towards mental well-being
Frequently Asked Questions (FAQs)
1. How do I know if what I’m experiencing is OCD or just overthinking?
It can be difficult to tell the difference. OCD typically involves persistent, intrusive thoughts along with a strong urge to perform certain behaviours to reduce anxiety. If it feels repetitive and hard to control, it may be worth seeking professional guidance.
2. Why do my thoughts feel so real and convincing?
In OCD, thoughts can feel highly intense and believable, even when you know logically they may not be true. This is because OCD attaches meaning and urgency to the thoughts, increasing anxiety.
3. Will CBT force me to face things I’m not ready for?
CBT is usually paced carefully and collaboratively. A therapist will work with you gradually, ensuring that any exposure feels manageable and supported rather than overwhelming.
4. Does avoiding triggers help with OCD?
Avoidance may reduce anxiety in the short term, but it often strengthens OCD over time. CBT helps individuals gently face triggers in a safe and structured way.
5. Will I always have OCD, or can it be managed long-term?
While OCD may not completely disappear for everyone, it can be effectively managed. With the right support and strategies, many people experience significant improvement and regain control over their lives.


